Article
Getmanenko Ya.A., Trusova A.V., Dobrovol’skaya A.E., Sofronov A.G. (2019). The influence of family system and individual psychological characteristics of the caregiver on the effectiveness of socio-psychological adaptation in patients with schizophrenia. National Psychological Journal, [Natsional’nyy psikhologicheskiy zhurnal], (12)3, 101–112
Abstract
Background. Family of schizophrenic patient plays a key role in their psychosocial adaptation. On the other hand, according to numerous data, adverse family relations are associated with high relapse risk. Family member’s illness is a severe stress factor for the whole family. However, families differ from each other to the degrees of emerging dysfunctions. Yet mechanisms which underlay interactional disturbances in those families remain unexplored.
Objective. The study represents complex research of the role of symptoms severity, interactional characteristics of a family, which are represented in family flexibility and cohesion parameters (FACES-3), and emotional and communicative competence (EmIn Lousin D.V.) as well as life satisfaction of main caregiver in psychosocial adaptation of a patient with schizophrenia.
Design. The paper presents the research of 122 test subjects, paired in dyads – schizophrenic patient (paranoid form) and their major caregiver. Patients gender distribution: 33 female and 28 males, average age 32.5±9.44 (M±SD), hospitalizations rate – 5.44 ±5.27, average illness duration – 9.93±6.85. Caregiver’s genders: 12 males and 49 females. Average major caregiver’s age – 53±11.91.
Results. Derived from structural equations, a model was invented showing that symptoms severity plays negative role in psychosocial adaptation of a patient with schizophrenia (p<0.001), whilst more balanced family characteristics have a supportive effect (p<0.001). Communicative competence of major caregiver increases balance of family characteristics (p<0.001).
Conclusion. The results indicate that the possibilities of social adaptation in patients with schizophrenia are determined by both objective factors (the severity of psychopathological symptoms) and the character of family dysfunctions that are closely associated with the emotional and communicative competence of main caregivers. In this way development of communicational skills in major caregivers may be the part of complex psychosocial interventions into schizophrenic patient’s families. Further research in this area may be aimed both at assessing the effectiveness of interventions, and at improving the tools to be used through experimental methods of assessing the family disruptions and emotional and communicative competence, as well as expanding the number of measured parameters (e.g. cognitive deficit of patients) for a more comprehensive understanding of the problem.
Accepted: 09/06/2019
Pages: 101-112
DOI: 10.11621/npj.2019.0311
PDF: Download
Keywords: schizophrenia; family interventions; expressed emotion; quality of life; family burden;
Available Online 20.10.2019
Acknowledgments
The paper is prepared under scientific project No. 17-29-02173 with financial support of the Russian Foundation for Basic Research (RFBR).
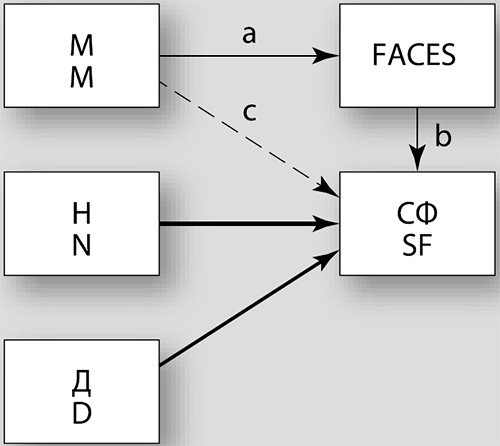
Fig. 1. Final model of the relationship of the individual-personality characteristics of the caregiver, family dynamics, severity of symptoms and social functioning of the patient
NB: SF - social functioning of the patient (PSP); N - negative symptoms (PANSS); D - other disorders (somatic) (PANSS); Ire - interpersonal EQ caregiver; FACES - medium balanced family type.
Bold (Red) highlighted negative effects, normal font (green) - positive; dashed line - lack of communication.
Table 1. Descriptive statistics of the clinical and psychological characteristics of the sample
|
Indicator |
N |
N (%) |
Mean |
SD |
Median |
q1 |
q3 |
|
PANSS Positive Symptoms |
- |
- |
13.46 |
3.53 |
13.0 |
11.0 |
16.0 |
|
PANSS Negative Symptoms |
- |
- |
23.74 |
7.18 |
25.0 |
18.0 |
30.0 |
|
PANSS Composite Index |
- |
- |
-10.33 |
6.43 |
-11.0 |
-14.0 |
-6.0 |
|
PANSS General somatic disorders |
- |
- |
30.49 |
8.14 |
29.0 |
24.0 |
36.0 |
|
PANSS Total |
- |
- |
67.66 |
16.03 |
66.0 |
55.0 |
80.0 |
|
PSP Patient |
- |
- |
58.48 |
16.13 |
59.0 |
47.0 |
71.0 |
|
QOL patient |
- |
- |
188.16 |
29.41 |
186.0 |
171.0 |
206.0 |
|
EQ patient interpersonal |
- |
- |
36.90 |
8.81 |
36.0 |
31.0 |
43.0 |
|
EQ patient intrapersonal |
- |
- |
44.28 |
10.50 |
44.0 |
37.0 |
53.0 |
|
EQ patient general |
- |
- |
81.18 |
17.71 |
80.0 |
68.0 |
91.0 |
|
LSI caregiver |
- |
- |
22.69 |
6.35 |
22.0 |
18.0 |
27.0 |
|
EQ interpersonal component caregiver |
- |
- |
39.52 |
6.61 |
39.0 |
34.0 |
43.0 |
|
EQ intrapersonal caregiver |
- |
- |
50.75 |
6.64 |
51.0 |
46.0 |
4.0 |
|
EQ total caregiver rate |
- |
- |
90.15 |
11.55 |
89.0 |
83.0 |
9.0 |
NB: N - absolute values; N (%) - fractions of the whole; Mean - arithmetic mean; SD - standard deviation; Median - median value; q1 - 25 percentile; q3 - 75 percentile/
Table 2. Comparison of EQ methodology data with standard indicators
|
Indicator |
Median |
q1 |
q3 |
U |
P |
|
EQ patient interpersonal |
3.0 |
1.0 |
5.0 |
261.0 |
<0.001 |
|
EQ patient intrapersonal |
5.0 |
4.0 |
7.0 |
778.5 |
0.277 |
|
EQ interpersonal caregiver |
4.0 |
2.0 |
5.0 |
215.5 |
<0.001 |
|
EQ intrapersonal caregiver |
7.0 |
6.0 |
8.0 |
1139.0 |
<0.001 |
Table 3. FACES-3 Method data
|
Unity Rate |
N |
N(%) |
|
Disunited |
42 |
68.85 |
|
Disjunct |
15 |
24.59 |
|
Connected |
4 |
6.56 |
|
Linked |
0 |
0 |
|
Adaptation Type |
N |
N(%) |
|
Rigid |
3 |
4.92 |
|
Structural |
5 |
8.2 |
|
Flexible |
9 |
14.75 |
|
Chaotic |
44 |
72.13 |
|
System Type |
N |
N(%) |
|
Medium balanced |
31 |
50.82 |
|
Unbalanced (extreme) |
30 |
49.18 |
Table 4. Descriptive table with a grouping factor "balance of the family system"
|
Indicator |
Unbalanced Type |
Balanced Type |
|
|||||||||
|
N |
% |
Mean |
SD |
N |
% |
Mean |
SD |
χ2
|
P |
log (odd) |
s.e. |
|
|
Female gender |
16 |
53 |
- |
- |
17 |
55 |
- |
- |
- |
- |
- |
- |
|
Male gender |
14 |
47 |
- |
- |
14 |
45 |
- |
- |
- |
- |
- |
- |
|
Age |
- |
- |
34 |
9.7 |
- |
- |
31 |
8.9 |
3.27 |
0.070 |
- |
- |
|
Number of hospitalizations |
- |
- |
6.1 |
5.9 |
- |
- |
4.8 |
4.7 |
0.62 |
0.430 |
- |
- |
|
Disease duration |
- |
- |
11 |
6.6 |
- |
- |
8.8 |
7.0 |
2.55 |
0.110 |
- |
- |
|
PANSS Positive Symptoms |
- |
- |
13 |
3.6 |
- |
- |
14 |
3.5 |
0.03 |
0.854 |
- |
- |
|
PANSS Negative Symptoms |
- |
- |
26 |
6.3 |
- |
- |
21 |
7.1 |
9.73 |
0.002 |
-1.52 |
0,49 |
|
PANSS Composite Index |
- |
- |
-13 |
5.7 |
- |
- |
-7.8 |
6.1 |
12.28 |
<0.001 |
1,75 |
0,50 |
|
PANSS Other Disturbances |
- |
- |
34 |
7.5 |
- |
- |
28 |
7.7 |
8.28 |
0.004 |
-1,36 |
0,47 |
|
PANSS Total |
- |
- |
73 |
15 |
- |
- |
62 |
15 |
7.64 |
0.006 |
-1,30 |
0,47 |
|
PSP Patient |
- |
- |
49 |
11 |
- |
- |
68 |
15 |
21.11 |
<0.001 |
2,51 |
0,55 |
|
QOL Patient |
- |
- |
180 |
24 |
- |
- |
196 |
32 |
5.29 |
0.021 |
1,07 |
0,46 |
|
EQ Patient Interpersonal |
- |
- |
35 |
7.9 |
- |
- |
39 |
9.4 |
1.65 |
0.198 |
- |
- |
|
EQ Patient Intrapersonal |
- |
- |
42 |
11 |
- |
- |
46 |
10 |
3.57 |
0.059 |
- |
- |
|
EQ Patient Total score |
- |
- |
77 |
17 |
- |
- |
85 |
17 |
3.94 |
0.047 |
0,92 |
0,46 |
|
LSI caregiver |
- |
- |
20 |
4.5 |
- |
- |
25 |
6.9 |
9.77 |
0.002 |
1,52 |
0,49 |
|
EQ Interpersonal caregiver |
- |
- |
36 |
5.6 |
- |
- |
43 |
5.3 |
25.16 |
<0.001 |
3,17 |
0,63 |
|
EQ Intrapersonal caregiver |
- |
- |
48 |
5.7 |
- |
- |
53 |
6.4 |
12.23 |
<0.001 |
1,72 |
0,49 |
|
EQ Total score caregiver |
- |
- |
83 |
9.4 |
- |
- |
97 |
9.7 |
20.42 |
<0.001 |
2,47 |
0,55 |
Table 5. Statistical Model Coefficients
|
Variables |
Model 1 |
Model 2 |
Final Model |
|
SF ~ P |
-0.017(0.050). z=-0.33. (p=0.742) |
-0.007(0.054). z=-0.13. (p=0.894) |
|
|
SF ~ N |
-0.069(0.029). z=-2.35. (p=0.019) |
-0.109(0.024). z=-4.50. (p<0.001) |
-0.094(0.016). z=-5.85. (p<0.001) |
|
SF ~ D |
-0.077(0.027). z=-2.88. (p=0.004) |
-0.050(0.023). z=-2.22. (p=0.026) |
-0.067(0.012). z=-5.67. (p<0.001) |
|
SF ~ Ire |
0.014(0.023). z=0.62. (p=0.536) |
-0.068(0.025). z=-2.67. (p=0.008) |
-0.003(0.008). z=-0.42. (p=0.675) |
|
SF ~ Ira |
-0.013(0.031). z=-0.42. (p=0.675) |
-0.030(0.028). z=-1.06. (p=0.289) |
|
|
SF ~ QOL |
0.033(0.032). z=1.03. (p=0.305) |
0.014(0.023). z=0.60. (p=0.546) |
|
|
SF ~ FACES |
0.926(0.409). z=2.26. (p=0.024) |
0.737(0.070). z=10.53. (p<0.001) |
0.556(0.065). z=8.50. (p<0.001) |
|
FACES ~ Ire |
|
0.164(0.027). z=6.07. (p<0.001) |
0.085(0.003). z=25.54. (p<0.001) |
|
FACES ~ Ira |
|
0.038(0.019). z=1.96. (p=0.050) |
|
|
FACES ~ QOL |
|
0.002(0.028). z=0.09. (p=0.928) |
|
|
Mediation:= a*b |
|
|
0.047(0.006). z=7.42. (p<0.001) |
|
total := c+a*b |
|
|
0.044(0.008). z=5.48. (p<0.001) |
|
chi |
χ²=0.000. df=38.000. p=1.000 |
χ²=65.630. df=42.000. p=0.011 |
χ²=26.366. df=41.000. p=0.963 |
|
rmsea |
0.000. p=1.000 |
0.097. p=0.059 |
0.000. p=0.990 |
|
srmr |
0.000 |
0.207 |
0.131 |
|
cfi |
1.000 |
0.000 |
1.000 |
References:
Albacete A., Bosque C., Custal N., Crespo J., Gilabert E., Albiach A., Menchón J., Contreras F. (2016) Emotional intelligence in non-psychotic first-degree relatives of people with schizophrenia. Schizophrenia Research, 175(1–3), 103–108. doi: 10.1016/j.schres.2016.04.039
Caqueo-Urízar, A., Rus-Calafell, M., Craig, T., Irarrazaval, M., Urzúa, A., Boyer, L., Williams, D.R. (2017) Schizophrenia: Impact on Family Dynamics. Current Psychiatry Reports, 19(1). doi: 10.1007/s11920-017-0756-z
Degnan, A., Baker, S., Edge, D., Nottidge, W., Noke, M., Press, C., Drake, R. (2018) The nature and efficacy of culturally-adapted psychosocial interventions for schizophrenia: A systematic review and meta-analysis. Psychological Medicine, 48(5), 714–727. doi: 10.1017/S0033291717002264
Eidemiller E.G., Dobryakov I.V., & Nikolskaya I.M. (2003). Family diagnosis and family psychotherapy. A manual for doctors and psychologists. SPb., Rech’.
Gurovich I.Ya., & Shmukler A.B. (2007). Workshop on psychosocial treatment and psychosocial rehabilitation of the mentally ill. Moscow, Medpraktika.
Kay S., Fiszbein A., Opler L. (1987) The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophrenia Bulleten, 13(2), 261–276. doi: 10.1093/schbul/13.2.261
Konovalova A.Kh., Kholmogorova A.B., & Dolnykova A.A. (2013). Representation of the parental family in patients with schizoaffective disorders and schizophrenia. [Konsul'tativnaya psikhologiya i psikhoterapiya, 4, 70–95.
Krasilnikova E.D., & Nikolskaya I.M. (2012). Psychological characteristics of a family raising children with different types of mental development disorders. [Klinicheskaya i spetsial'naya psikhologiya], 4. Retrieved from: http://psyjournals.ru/psyclin/2012/n4/57308.shtml (accessed March 16, 2019).
Kulhara P, Kate N, Grover S, Nehra R. (2013) Positive aspects of caregiving in schizophrenia: A review. World Joutnal of Psychiatry, 2(3), 43–48. doi: 10.5498/wjp.v2.i3.43
Lauber C., Eichenberger A., Luginbuhl P., Keller C., Rossler W. (2003) Determinants of burden in caregivers of patients with exacerbating schizophrenia. European Psychiatry, 18, 285–289. doi: 10.1016/j.eurpsy.2003.06.004
Lavoie M., Plana I., Bédard Lacroix J., Godmaire-Duhaime F., Jackson P., Achim A. (2013) Social cognition in first-degree relatives of people with schizophrenia: a meta-analysis. Psychiatry Research, 209(2), 129–35. doi: 10.1016/j.psychres.2012.11.037
Lyusin D.V. (2006). A new methodology for measuring emotional intelligence: Emin questionnaire. [Psikhologicheskaya diagnostika], 4, 3–22.
Macgregor A., Norton J., Raffard S., Capdevielle D. (2017) Is there a link between biological parents' insight into their offspring's schizophrenia and their cognitive functioning, expressed emotion and knowledge about disorder? Comprehensive Psychiatry, 76, 98–103. doi: 10.1016/j.comppsych.2017.02.013
Martens L., Addington J. (2001) The psychological well-being of family members of individuals with schizophrenia. Social Psychiatry and Psychiatric Epidemiology, 36(3), 128–133. doi: 10.1007/s001270050301
Martorell A., Pereda A., Salvador-Carulla L., Ochoa S., Ayuso-Mateos J. (2007) Validation of the Subjective and Objective Family Burden Interview (SOFBI/ECFOS) in primary caregivers to adults with intellectual disabilities living in the community. Journal of Intellectual Disability Research, 51(11), 892–901. doi: 10.1111/j.1365-2788.2007.00962.x
Maslovsky S.Yu., & Kozlovsky V.L. (2009). Measurement of the quality of life of patients with schizophrenia during maintenance therapy. [Obozrenie psikhiatrii i meditsinskoy psikhologii im. V.M. Bekhtereva], 3, 29–32.
Morosini P., Magliano L., Brambilla L., Ugolini S., Pioli R. (2000) Development, reliability and acceptability of a new version of the DSM-IV Social and Occupational Functioning Assessment Scale (SOFAS) to assess routine social functioning. Acta Psychiatrica Scandinaviсa, 101(4), 323–329. 10.1111/j.1600-0447.2000.tb10933.x
Olson D. (2000) Circumplex Model of Family Systems. Journal of Family Therapy, 22 (2), 144–167. doi: 10.1111/1467-6427.00144
Pakenham K., Chiu J., Bursnall S., Cannon T. (2007) Relations between social support, appraisal and coping and both positive and negative outcomes in young carers. Journal of Health Psychology, 12(1), 89–102. doi: 10.1177/1359105307071743
Panina N.V. (1993). Life Satisfaction Index. [LifeLine i dr. novye metody psikhologii zhiznennogo puti]. Moscow, Progress-Kultura, 107–114.
Parabiaghi A., Lasalvia A., Bonetto C., Cristofalo D., Marrella G., Tansella M., Ruggeri M. (2007) Predictors of changes in caregiving burden in people with schizophrenia: A 3-year follow-up study in a community mental health service. Acta Psychiatrica Scandinavica, 437, 66–76. doi: 10.1111/j.1600-0447.2007.01094.x
Pashkovsky V.E., Sofronov A.G., Fedorovsky I.D., & Dobrovolskaya A.E. (2017). Comparative analysis of indicators of social adaptation of patients with paranoid schizophrenia with frequent hospitalization. [Sotsial'naya i klinicheskaya psikhiatriya], 3 (27), 19–25.
Rychkova O.V. (2013). Studies of public knowledge in schizophrenia. [Konsul'tativnaya psikhologiya i psikhoterapiya], 1, 63–89.
Rychkova O.V., & Kholmogorova A.B. (2014). Main theoretical approaches to the study of violations of public cognition in schizophrenia: current status and development prospects [Konsul'tativnaya psikhologiya i psikhoterapiya], 22(4), 30–43.
Seeman M. (2009) The changing role of mother of the mentally ill: From schizophrenogenic mother to multigenerational caregiver. Psychiatry: Interpersonal and Biological Processes, 72(3), 284–294. doi: 10.1521/psyc.2009.72.3.284
Sofronov A.G., Pashkovsky V.E., Dobrovolskaya A.E., & Fedorovsky I.D. (2018). Description of environmental pathoplastic factors in the clinical picture of schizophrenia. [Meditsinskiy akademicheskiy zhurnal], 1(18), 45–55.
Veltman A., Cameron J., Stewart D. (2002) The experience of providing care to relatives with chronic mental illness. Journal of Nervous and Mental Disoders, 190, 108–114. doi: 10.1097/00005053-200202000-00008
Wang X., Chen Q., Yang, M. (2017) Effect of caregivers’ expressed emotion on the care burden and rehospitalization rate of schizophrenia. Patient Preference and Adherence, 11, 1505–1511. doi: 10.2147/PPA.S143873
Wearden A., Tarrier N., Barrowclough C., Zastowny T., Rahill A. (2000) A review of expressed emotion research in health care. Clinical Psychology Review, 20(5), 633–666. doi: 10.1016/S0272-7358(99)00008-2
Zvereva N.V., & Roshchina I.F. (2012). Family problems in clinical psychology. [Klinicheskaya i spetsial'naya psikhologiya, 1. Retrieved from: http://psyjournals.ru/psyclin/2012/n1/49967.shtml (accessed March 16, 2019).For citing this article:
Getmanenko Ya.A., Trusova A.V., Dobrovol’skaya A.E., Sofronov A.G. (2019). The influence of family system and individual psychological characteristics of the caregiver on the effectiveness of socio-psychological adaptation in patients with schizophrenia. National Psychological Journal, [Natsional’nyy psikhologicheskiy zhurnal], (12)3, 101–112


